I was 25-years old and staring death in the face. My leg hurt and I had difficulty walking, but I otherwise felt and looked healthy. No one would have guessed that I could easily drop dead at a second’s notice. I was young and in relatively good shape. In the past year, I’d run two half-marathons and I was now in the middle of a month-long backpacking trip through Southeast Asia with my friends.
But I somehow ended up on a seven-hour flight from Malaysia to Tokyo, alone, and seriously wondering if I would make it to my 26th birthday the following week. Three days earlier, I had been diagnosed with deep vein thrombosis (DVT) in Kuala Lumpur, nearly ten thousand miles away from home, and although I didn’t know it, I had already developed pulmonary embolisms (PEs).
I want to tell my story in the hopes that you will learn the signs of this potentially fatal condition. It is often left undiagnosed and is incredibly serious. DVT/PEs can affect and kill almost anyone in any age group and in any state of health. You may have heard of NBC’s David Bloom, 39, who died unexpectedly while reporting in Iraq. Or you may have heard of teenagers dying unexpectedly after playing video games for days without stopping. Or you may have heard that Hilary Clinton suffered her own DVT scare in 1998. There are countless stories.
My hope is that if you learn the risk factors and symptoms, you, your family, and your friends will be able to avoid a similar debacle.
—
DVT occurs when a blood clot develops in a vein and begins to block the blood flow back to your heart. It often occurs in the lower leg, thigh or pelvis, but can also develop in the arm.
What makes a DVT so dangerous is that a part of this clot can break off and travel through the vein, through the heart and into the lungs. The DVT then becomes a PE, which can stop blood from reaching the lungs—if the clot is big enough, you die.

This scan of my leg shows that my left leg (right in this image) is swollen.
In most cases, the DVT is small and limited to one area. Regardless, a blood clot of any size can break off, and if the piece is large enough, it can be deadly.
In my case, the DVT was severe. My entire left leg, through my pelvis, and nearly all the way to my heart was one enormous blood clot. In half of the cases that are this serious, the patient either dies or loses the leg.
Because my prognosis was so grave, and because the medical care in Malaysia was insufficient, I flew to Tokyo, despite the risks, on the recommendation of my friend’s father (an ER doctor). By the time I landed in Tokyo and was rushed into the ICU and surgery, they discovered that I already had several PEs. I had been lucky they were small.
—
Each year DVT/PEs kill more than 300,000 people in the U.S.—more than HIV and breast cancer combined. However, DVT can be treated and PEs prevented if discovered early.
Hanging out in the hostel. Unable to walk, but it would be days before I knew what was wrong.
We had been traveling through Southeast Asia for three weeks, and I had been having lower back pain for about a week. I didn’t think much of it and chalked it off to the uncomfortable beds in our cheap hostels. On our last night in Kuala Lumpur, my left leg started to swell unexpectedly. Within a couple hours the pain and swelling were so severe that I could no longer walk. My leg became discolored and for the next two days my roommate and I went to different hospitals in order to get a diagnosis—all the while my leg became progressively darker, and the pain increasingly crippling. Although DVT symptoms are commonly recognized by American doctors, I had a hard time getting answers in Malaysia. At one point one of the doctors told me to go back to my country to get my leg fixed. Eventually, I was able to convince one of the doctors to give me a scan after my foot started to turn blue, revealing that I had a DVT.
It is important to know the signs of a DVT so that you can seek medical help immediately:
- Swelling
- Pain
- Tenderness
- Discoloration or redness of skin
- Warm skin

My left leg (right in this image) was starting to turn blue when the doctor finally agreed to give me a scan.
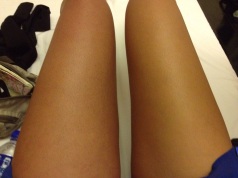
My left leg was swollen, darker and in excruciating pain.
You can also develop a PE without showing DVT symptoms. You should go to the hospital immediately if you have these symptoms:
- Difficulty breathing
- Faster than normal or irregular heart beat
- Chest pain or discomfort, which usually worsens with a deep breath or coughing
- Coughing up blood
- Very low blood pressure, lightheadedness, or fainting
—
What makes this so scary is that half the time, people show no symptoms of a DVT at all. It is therefore important to know what causes a DVT, and also know what you can do to prevent a DVT from happening in the first place.
Anyone can have a DVT, but your odds increase with each risk factor present:
- Sitting for long periods without moving (long plane flights and car rides)
- Birth control pills (or other increases in estrogen, including pregnancy and HRT)
- Smoking
- Surgery
- Obesity
- Cancer
- Heart and lung disease
- Genetic clotting disorders
- Age > 40
- Previous history of DVT/PE in you or your family

I looked OK. But I would spend another 6 weeks in a wheelchair. And it would be another 4 months before I could walk more than a few blocks.
It is likely that I had been a walking time bomb for three weeks, and could have died at any given moment during our trip. I had flown to Thailand at the end of July and subsequently sat through three long flights to Bangkok. I was exhausted and dehydrated from a weekend of celebrating the end of the bar exam and I slept the entirety of each plane ride, walking only to transfer in between flights.
I later found out that I had two other risk factors, which greatly increased my odds of developing a DVT—I was on birth control and have a genetic condition called Factor V Leiden, which makes my blood thicker than the average person (1 in 20 Caucasians has this). It is likely that my clot started out small and grew larger as more and more of my blood flow became blocked, which is why my DVT was so extensive by the time I finally started showing symptoms.
—
Being abroad complicated my situation dramatically. I did not receive treatment that was aggressive enough and as a result, I will have to live with my DVT as a lifelong disability. I have an 8-inch stent (metal vein) in my pelvis, have completely lost my deep left thigh vein because the blood clot is now permanent scar tissue, am on an impressive arsenal of blood thinners, and am forced to wear a full-length compression stocking on my left leg (very trendy fashion statement) to help prevent the blood from pooling.
I spent a total of 6 weeks in 4 hospitals around the globe, spent 3 weeks hooked up to an IV, and have had 7 surgeries (and counting). Exactly a year ago I could not walk. Nine months ago I was told that I would have to accept that I would never run long distances again.
I say all this to those of you who have experienced a DVT. Your body is an incredible machine, and it can recover, even if your DVT is as severe as mine. After pushing my body to its limits—going to the gym regularly, engaging in strength training, and just running through the excruciating levels of pain—I can run again. I completed my first post-legscapade half marathon in May and will run another this October. Next up, I’ll be training to run the November 2014 NYC marathon.
Although I have worked hard to build my body back to the level it is now, I also recognize that there was an enormous amount of luck that played a role in my still being here today. But you don’t need luck to prevent a DVT—you just need to remember simple preventative tips. Before a long flight, take an aspirin. Make sure to move around during the flight. Stay hydrated. The same goes for a long car ride or any situation where you will be sitting for a long period of time. My story would have turned out differently had I known these things. Don’t let the same happen to you.
I’m running the NYC Marathon to help STOP THE CLOT for the National Blood Clot Alliance. If you’d like to help, please donate HERE. Thank you!











