I successfully completed all my runs this week, and it’s clear this summer humidity is going to be a real challenge–but one that I’m willing to tackle!
I’ve always been a fan of summer, and I will take the worst of NYC heat and humidity over winter any day. But even so, it makes it very difficult to run.
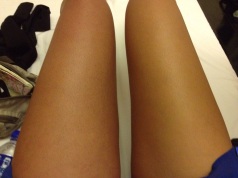
I wear a compression stocking on my left leg that goes up to my thigh. As far as I know, it’s something I’ll need to wear for the rest of my life. It’s basically a very tight sock that combats swelling by helping keep the blood from pooling in my leg (blood goes in just fine, but because my veins are clogged, it’s difficult for the blood to leave).
Unfortunately, the compression stocking makes it hard for my leg to breathe. The stocking is so tight, I can’t sweat out of that leg, and I quickly overheat. The humidity is brutal. I hope that by powering through, these runs will eventually get easier. And when the November NYC Marathon rolls around, I’ll have some extra preparation!
Even though my initial diagnosis of the deep vein thrombosis (DVT) is nearly two years behind me, it’s still difficult to deal with the consequences of the clot in my leg being permanent.
I don’t believe in living life by saying “If only…” or “I wish I’d known…,” but if I had known one thing, it would have completely changed my life and leg.
A DVT will become permanent scar tissue if it is not properly dealt with in the first few weeks.
Most of the time, this is not a problem. Doctors use two main treatments to treat a DVT.
- Blood thinners: In most cases, blood clots are small (but deadly) and can be treated with anticoagulants (blood thinners). These drugs increase the amount of time it takes for a blood clot to form and allow your body to naturally take care of the existing clot.
- Clot-busters: In cases of more extreme DVT, the body alone is unable to clear the clot by itself. A clot-busting drug can be injected directly into the blood stream or the clot to help the body “melt” the clot away at a much faster rate.
Unfortunately, in my case, I had the perfect storm of problems. My DVT was extremely severe (phlegamasia cerulea dolens) and went from my ankle to my heart. It was so bad my foot was turning blue. I had a 50% chance of dying or losing my leg. I also got sick in Malaysia, meaning I did not have access to modern healthcare.
The doctors in Malaysia were satisfied with treating me exclusively with a blood thinner (xarelto, which I’m on today). Despite the severity of my DVT, they opted to go with the standard treatment of blood thinners—only effective in less extreme cases—and to let my body essentially take care of the clot itself.
It’s safe to say, had I stayed in Malaysia, I’d either be dead or short a left leg. There is no way my body could have tackled a four-foot long blood clot on its own.
After a couple nights, I flew to Tokyo to seek more advanced treatment. The doctors in Tokyo were much more prepared to handle a DVT of my severity, and within a couple hours of landing in Tokyo, I was in the operating room receiving a filter to catch blood clots before they could enter my heart lungs (inferior vena cava filter/IVC filter).
They chose to treat my DVT by hooking me up to an IV and filling my blood stream with the clot-busting drugs (urokinase). Although they considered injecting the clot-busting drug directly into my clot (catheter directed thrombolysis), there is a risk of severe and fatal bleeding. This was not a common procedure in Japan, and they decided to play it safe.
It would take longer, but my body would take care of the clot over the next few months with the help of the clot-busting drug. Patience would pay off.
I spent a month in the hospital in Tokyo. I was not allowed to go outside, I could not walk, and I was hooked up to an IV. The clot-busting drug was slowly but surely effective. My weekly MRIs showed the clots in my lungs (pulmonary embolisms) and in my lower leg and mid-section “melting” away, and the clot that had extended from my ankle to my heart gradually became shorter.
Unfortunately, the clot-busting medication never got a chance to “melt” the vast majority of my clot. My upper calves, my thigh, my pelvis—none of these were exposed to the medication because blood flow in the area was so poor. Only the peripheral clots were exposed to the clot-busting drug in my blood stream. The majority of my DVT was left untreated.
Five weeks after my initial diagnosis, I flew back to New York to finish treatment. It was here that I learned a DVT will become permanent scar tissue if it is not properly dealt with in the first few weeks.
What I hadn’t known was that I had been sitting in various hospitals in Asia, waiting patiently, and quietly allowing all of my blood clots to become permanent scar tissue. I had passively sat around, and with each passing day, I ensured a lifelong disability with lifelong poor circulation.
If only I had known.
It had already been five weeks, but the doctors in New York tried injecting the clot-busting drugs (rTPA) directly into my leg (catheter directed thrombolysis). Small portions of the clot (likely new clots resulting from my poor circulation) “melted” away, but ultimately it was ineffective.
The deep veins in my leg were left permanently scarred and blocked.
It’s easy to go back and wonder about how things would be different if my DVT had been less severe, if I had gotten sick in America, if I’d only gone back to New York earlier, or if I’d known I had a limited window of time…
Had I known, I would have flown back to NYC as soon as I had the IVC filter (to catch blood clots) inserted in Tokyo.
Had I known, I would have asked for more aggressive treatment and catheter directed thrombolysis.
Had I known, I would have busted the clots before they became permanent.
…but ultimately, this does no good. It might have been a lot worse. I’m alive, I’m running, and I don’t plan on letting DVT stop me from anything.
Please be mindful of your treatment—you only have a limited time to bust the clot before it becomes permanent. Consult your doctor and get a second and third opinion.
No one cares more about your well-being and treatment than you.